Monisha Chrishaille 1 , Akilandeswari Manickam 2 , Rajesh Kumar Kodali 3
Author affiliations:
Background: Odontogenic infections that extend into the cervicofacial and periorbital regions can create a critical airway challenge. Marked swelling and trismus frequently distort the anatomy, making bag–mask ventilation unreliable and complicating laryngoscopy. In this setting, induction of general anesthesia carries the risk of losing both ventilation and intubation. An awake approach that preserves spontaneous breathing and ensures continuous oxygenation provides a safer path to airway control.
Case Presentation: A 61-year-old woman developed progressive left facial and periorbital swelling with abscess formation two days after dental extraction. On arrival, she had severe trismus, with an interincisor distance of about 1.5 cm. The team planned an awake intubation. Topical anesthesia was achieved using 4% lidocaine in multiple forms, and dexmedetomidine was titrated to maintain cooperative sedation (RASS −2 to −1). High-flow nasal oxygen was delivered via high-flow nasal oxygen, starting at 30 L/min and increased to 60 L/min with FiO₂ 1.0, maintained throughout preparation and laryngoscopy. Using a C-MAC videolaryngoscope with a hyper-angulated blade, a partial but adequate view of the glottis (POGO 60–70%) was obtained. A bougie was advanced under direct vision, and a 7.0-mm cuffed endotracheal tube was successfully railroaded on the first attempt. Oxygen saturation remained ≥98% with stable hemodynamics. The abscess was surgically drained, and the patient was extubated safely after 36 hours. She was discharged home on the fifth postoperative day in good condition.
Conclusion: For patients with airway compromise due to infective trismus, awake videolaryngoscopy supported by continuous high-flow nasal oxygenation and planned use of adjuncts such as a bougie can facilitate controlled, atraumatic intubation. This combination minimizes the risk of desaturation and maximizes the chance of first-pass success
Keywords: Facial cellulitis; difficult airway; videolaryngoscopy; high-flow nasal oxygenation; awake intubation; multidisciplinary airway management
Citation: Chrishaille M, Manickam A, Kodali RK. Awake videolaryngoscopy with high-flow nasal oxygenation for odontogenic facial–periorbital cellulitis with abscess and trismus: a case report. Anaesth. pain intensive care 2026;30(1):124-128. DOI: 10.35975/apic.v30i1.3087
Received: August 02, 2025; Revised: September 27, 2025; Accepted: January 18, 2026
Odontogenic infections can spread quickly along cervicofacial fascial planes, leading to trismus, soft-tissue swelling, and deformation of the upper airway. Once the process extends into the periorbital region, the clinical challenge increases: not only may vision be at risk, but the airway itself becomes more complex to manage. In such situations, both mask ventilation and laryngoscopy can be unreliable, and the safe window for securing the airway before desaturation is often very short. These patients therefore require an anticipatory strategy that maintains oxygen delivery and permits careful, deliberate airway manipulation.
For patients with a predicted difficult airway, the guiding principles remain the same: spontaneous breathing should be preserved, topical anesthesia must be thorough, and desaturation-driven haste should be avoided. Awake tracheal intubation (ATI) is widely regarded as the preferred approach when difficulty with mask ventilation or intubation is expected.1,2 Videolaryngoscopy (VL) and flexible bronchoscopy are both valid options; the choice is shaped by clinician experience, anatomical considerations, and the intended route of access. Regardless of the device, the essential elements are adequate topicalization, controlled sedation, and continuous oxygenation.
Oxygenation strategy has become a key modifiable factor in airway safety. High-flow nasal oxygen (HFNO), also known as transnasal humidified rapid insufflation ventilatory exchange (THRIVE), delivered through the THRIVE technique, provides warmed, humidified gas at high flows (up to ~70 L/min). This supports apnoeic oxygenation, contributes a small degree of positive airway pressure, and assists with carbon dioxide clearance, thereby extending the apnoea time available during airway interventions.3,4 THRIVE is particularly advantageous in patients with severe trismus or when prolonged laryngoscopy is anticipated.
The supporting evidence includes physiological studies, controlled trials, and systematic reviews. Early investigations demonstrated increased oxygen reserves and longer apnea tolerance compared to conventional preoxygenation.5,6 More recent data confirm that, although HFNO does not eliminate every episode of desaturation, it consistently improves oxygenation, ensures uninterrupted oxygen delivery during instrumentation, and expands the safe procedural window—advantages that are most valuable when intubation is technically complex.7,8 Current airway guidelines also emphasize the need for sustained oxygenation throughout preparation, intubation, and early recovery.
In cases of cervicofacial infection with trismus, VL offers clear practical advantages. With the camera located at the blade tip, VL reduces the requirement to align airway axes, enabling improved glottic exposure in swollen or crowded upper airways. The shared view also allows team members to assist with maneuvers such as suction, external laryngeal pressure, or adjunct placement. When VL is integrated with awake ATI principles and supported by THRIVE, intubation can be performed in a structured, stepwise manner that reduces reliance on rescue ventilation and minimizes the risk of hypoxemia.
Within this framework, we describe a 61-year-old woman with odontogenic facial–periorbital cellulitis and abscess associated with severe trismus, successfully managed with awake videolaryngoscopy (C-MAC) and continuous para-oxygenation via THRIVE. This case demonstrates how combining established ATI principles with VL and HFNO widens the margin of safety and facilitates controlled, first-pass success in a high-risk airway.
A 61-year-old woman presented after 48 hours of rapidly progressive left-sided facial swelling and pain following a dental extraction, with fever and reduced oral intake. The swelling had tracked superiorly into the periorbital region(Figure 2A). She was alert and cooperative. Vital signs: blood pressure 132/78 mmHg, heart rate 102 beats/min, respiratory rate 18 / min, temperature 37.8 °C, and SpO₂ 98% on room air. Examination showed marked facial and periorbital edema with erythema and tenderness. Mouth opening was severely restricted (interincisor distance ≈ 1.5 cm; Figure 2B). Airway assessment identified Mallampati IV, thyromental distance 5.5 cm, and pain-limited neck extension, with no stridor and no drooling. Laboratory tests demonstrated leukocytosis with elevated inflammatory markers. Contrast-enhanced CT of the face and neck revealed diffuse soft-tissue edema and a localized abscess-centered in the left buccal/periorbital region, without deep-neck space extension or airway deviation. Key clinical and airway features are summarized in Table 1.
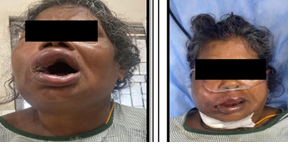
Figure 1: Clinical photographs at presentation and after intervention. (A) Left-sided facial swelling extending to the periorbital region, with restricted mouth opening (trismus ≈ 1.5 cm) with lip oedema. (B) Postoperative appearance after surgical drainage and airway stabilization
Given the predictors of a difficult airway—severe trismus, edema, and distorted anatomy—a multidisciplinary plan was agreed with the anesthesia and otolaryngology teams. The primary strategy was awake tracheal intubation using videolaryngoscopy, with flexible bronchoscopy and front-of-neck access prepared as contingency options.
In the operating room, standard monitoring (ECG, non-invasive blood pressure, pulse oximetry, capnography) was applied. High-flow nasal oxygen (THRIVE) was initiated at 30 L/min and escalated to 60 L/min with FiO₂ 1.0 to provide both preoxygenation and continuous paraoxygenation. The airway was topicalized with 4% lidocaine (lignocaine) using nebulization, sprays, and soaked swabs (total dose kept within safety limits). An intravenous dexmedetomidine infusion was titrated to cooperative sedation (RASS −2 to −1) while preserving spontaneous ventilation.
Videolaryngoscopy with a C-MAC hyperangulated blade yielded an adequate glottic view (POGO ~60–70%). A bougie was advanced under vision, and a 7.0-mm cuffed endotracheal tube was railroaded into the trachea. Intubation was successful on the first attempt without desaturation; SpO₂ remained ≥98% throughout and hemodynamics were stable.
Definitive management consisted of surgical drainage of the abscess and intravenous antibiotics. The patient was admitted to the ICU for observation and ventilatory support. With reduction in facial edema, she was extubated at 36 hours (Figure 1B) and subsequently recovered uneventfully, allowing discharge on postoperative day 5 in good condition.
Marked left-sided facial swelling extending into the periorbital region was evident on presentation. The patient had a severely restricted interincisor gap of ~1.5 cm (Figure 1A), limiting both airway evaluation and the feasibility of conventional laryngoscopy. These findings indicated a high risk of difficult mask ventilation and tracheal intubation. Awake videolaryngoscopic intubation with paraoxygenation was successfully performed, followed by surgical drainage of the abscess and postoperative management in the ICU. Over the next 36 hours, facial swelling subsided and the airway stabilized (Figure 1B). She was extubated safely and discharged on postoperative day five with full clinical recovery.
Odontogenic infections that extend into the cervicofacial and periorbital spaces create an urgent airway challenge. The combined effect of soft tissue swelling and severe trismus reduces the effectiveness of mask ventilation, limits maneuverability of airway devices, and leaves only a narrow margin for safe intervention. In these circumstances, preserving spontaneous breathing and opting for an awake approach helps to avoid the dangers of losing the airway after induction of anesthesia.9,10 In the present case, the use of comprehensive topicalization, carefully titrated dexmedetomidine sedation, videolaryngoscopy (VL) with a hyperangulated blade, pre-selected adjuncts, and continuous HFNO allowed a controlled, first-pass intubation with stable oxygenation and an uneventful recovery.11,12
The choice of airway device was a decisive factor. VL is consistently associated with better glottic exposure and higher first-pass success compared with direct laryngoscopy, particularly in difficult or infected airways. These benefits reduce the likelihood of escalation to rescue devices or surgical airway creation. Hyperangulated blades provide further advantage in situations where swelling and restricted mouth opening distort landmarks. However, a good laryngeal view alone does not always ensure successful tube passage. By intentionally pairing VL with a bougie introducer, the intubation in this case translated a satisfactory view into successful first-pass placement. This strategy is supported by both randomized trials and pooled analyses that emphasize the benefit of combining hyperangulated VL with an introducer to improve tube delivery.13–14
Oxygenation strategy was equally critical. Conventional preoxygenation provides only a limited safety window if laryngoscopy is prolonged. HFNO addresses this limitation by maintaining continuous oxygen delivery, generating a modest positive airway pressure, and facilitating gas exchange. Evidence from meta-analyses has demonstrated that this approach not only improves oxygenation but also extends the apnea time during difficult or rapid intubations, without increasing aspiration risk.In our patient, continuous HFNO during preparation and laryngoscopy ensured oxygen saturation remained ≥ 98%, eliminating time pressure and allowing an unhurried and atraumatic intubation.
Successful outcomes in cases of infective trismus also rely on process and preparedness. A multidisciplinary plan involving both anesthesiology and otolaryngology, with backup strategies such as flexible bronchoscopy and front-of-neck access, aligns with recommended practice in complex cervicofacial infections. This redundancy converts uncertainty into contingency rather than crisis and may explain why VL-first approaches in orofacial infection cohorts have been associated with lower rates of emergent tracheostomy. In our case, the course—first-pass success without desaturation, prompt surgical drainage, and early extubation—reflects the trajectory of improved outcomes highlighted in recent literature (see Supplementary Table S1 for study-level details.11–14
It is important to acknowledge the limitations of this report. Being a single case, outcomes were influenced by operator expertise, the team’s familiarity with awake VL, and access to equipment such as HFNO and bougies. In less well-resourced settings, awake flexible bronchoscopy remains a reliable alternative, while optimized facemask preoxygenation with nasal oxygen supplementation can substitute for HFNO, though with a narrower oxygenation margin. Nevertheless, the reproducible features supported by current evidence—choosing VL as the first-line tool for anticipated difficulty, routine use of adjuncts, continuous oxygen delivery, and preparation of rescue strategies—form a practical template for managing similar infected airways.
Airway management in cervicofacial infection with trismus is high risk, but structured planning and integration of contemporary techniques can substantially mitigate that risk. Awake VL, supported by meticulous topicalization, judicious sedation, adjunctive devices, and continuous oxygen delivery, provides a controlled pathway to first-pass success. This case underscores that effective management rests not on a single device or drug, but on coherently combining multiple evidence-based elements within a prepared, multidisciplinary team.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
7. Ethical considerations
Images de-identified with periorbital masking; written consent for clinical use and publication was obtained.
8. Authors’ contribution
MC: Conduct of case management, literature review, initial manuscript drafting
AM: Supervision of clinical procedures, critical review of manuscript, literature analysis
RKKV: Conceptualization, oversight of entire study, manuscript editing and correspondence
Author affiliations:
- Monisha Chrishaille, MD, Resident, Department of Anesthesiology, Sri Ramachandra Medical College and Research Institute, Chennai – 600 116, Tamil Nadu, India; Email: monishachrishaille@gmail.com; ORCID iD: {0009-0001-3740-352x}
- Akilandeswari Manickam, MD, Professor, Department of Anesthesiology, Sri Ramachandra Medical College and Research Institute, Chennai – 600 116, Tamil Nadu, India; Email: makilandeswari@yahoo.com; ORCID: {0000-0003-4576-391x}
- Rajesh Kumar Kodali V, MD, Professor, Department of Anesthesiology, Sri Ramachandra Medical College and Research Institute, Chennai – 600 116, Tamil Nadu, India; Email: vrajesh.kodali@gmail.com; ORCID iD: {0000-0002-4467-6657}
ABSTRACT
Background: Odontogenic infections that extend into the cervicofacial and periorbital regions can create a critical airway challenge. Marked swelling and trismus frequently distort the anatomy, making bag–mask ventilation unreliable and complicating laryngoscopy. In this setting, induction of general anesthesia carries the risk of losing both ventilation and intubation. An awake approach that preserves spontaneous breathing and ensures continuous oxygenation provides a safer path to airway control.
Case Presentation: A 61-year-old woman developed progressive left facial and periorbital swelling with abscess formation two days after dental extraction. On arrival, she had severe trismus, with an interincisor distance of about 1.5 cm. The team planned an awake intubation. Topical anesthesia was achieved using 4% lidocaine in multiple forms, and dexmedetomidine was titrated to maintain cooperative sedation (RASS −2 to −1). High-flow nasal oxygen was delivered via high-flow nasal oxygen, starting at 30 L/min and increased to 60 L/min with FiO₂ 1.0, maintained throughout preparation and laryngoscopy. Using a C-MAC videolaryngoscope with a hyper-angulated blade, a partial but adequate view of the glottis (POGO 60–70%) was obtained. A bougie was advanced under direct vision, and a 7.0-mm cuffed endotracheal tube was successfully railroaded on the first attempt. Oxygen saturation remained ≥98% with stable hemodynamics. The abscess was surgically drained, and the patient was extubated safely after 36 hours. She was discharged home on the fifth postoperative day in good condition.
Conclusion: For patients with airway compromise due to infective trismus, awake videolaryngoscopy supported by continuous high-flow nasal oxygenation and planned use of adjuncts such as a bougie can facilitate controlled, atraumatic intubation. This combination minimizes the risk of desaturation and maximizes the chance of first-pass success
Keywords: Facial cellulitis; difficult airway; videolaryngoscopy; high-flow nasal oxygenation; awake intubation; multidisciplinary airway management
Citation: Chrishaille M, Manickam A, Kodali RK. Awake videolaryngoscopy with high-flow nasal oxygenation for odontogenic facial–periorbital cellulitis with abscess and trismus: a case report. Anaesth. pain intensive care 2026;30(1):124-128. DOI: 10.35975/apic.v30i1.3087
Received: August 02, 2025; Revised: September 27, 2025; Accepted: January 18, 2026
1. INTRODUCTION
Odontogenic infections can spread quickly along cervicofacial fascial planes, leading to trismus, soft-tissue swelling, and deformation of the upper airway. Once the process extends into the periorbital region, the clinical challenge increases: not only may vision be at risk, but the airway itself becomes more complex to manage. In such situations, both mask ventilation and laryngoscopy can be unreliable, and the safe window for securing the airway before desaturation is often very short. These patients therefore require an anticipatory strategy that maintains oxygen delivery and permits careful, deliberate airway manipulation.
For patients with a predicted difficult airway, the guiding principles remain the same: spontaneous breathing should be preserved, topical anesthesia must be thorough, and desaturation-driven haste should be avoided. Awake tracheal intubation (ATI) is widely regarded as the preferred approach when difficulty with mask ventilation or intubation is expected.1,2 Videolaryngoscopy (VL) and flexible bronchoscopy are both valid options; the choice is shaped by clinician experience, anatomical considerations, and the intended route of access. Regardless of the device, the essential elements are adequate topicalization, controlled sedation, and continuous oxygenation.
Oxygenation strategy has become a key modifiable factor in airway safety. High-flow nasal oxygen (HFNO), also known as transnasal humidified rapid insufflation ventilatory exchange (THRIVE), delivered through the THRIVE technique, provides warmed, humidified gas at high flows (up to ~70 L/min). This supports apnoeic oxygenation, contributes a small degree of positive airway pressure, and assists with carbon dioxide clearance, thereby extending the apnoea time available during airway interventions.3,4 THRIVE is particularly advantageous in patients with severe trismus or when prolonged laryngoscopy is anticipated.
The supporting evidence includes physiological studies, controlled trials, and systematic reviews. Early investigations demonstrated increased oxygen reserves and longer apnea tolerance compared to conventional preoxygenation.5,6 More recent data confirm that, although HFNO does not eliminate every episode of desaturation, it consistently improves oxygenation, ensures uninterrupted oxygen delivery during instrumentation, and expands the safe procedural window—advantages that are most valuable when intubation is technically complex.7,8 Current airway guidelines also emphasize the need for sustained oxygenation throughout preparation, intubation, and early recovery.
In cases of cervicofacial infection with trismus, VL offers clear practical advantages. With the camera located at the blade tip, VL reduces the requirement to align airway axes, enabling improved glottic exposure in swollen or crowded upper airways. The shared view also allows team members to assist with maneuvers such as suction, external laryngeal pressure, or adjunct placement. When VL is integrated with awake ATI principles and supported by THRIVE, intubation can be performed in a structured, stepwise manner that reduces reliance on rescue ventilation and minimizes the risk of hypoxemia.
Within this framework, we describe a 61-year-old woman with odontogenic facial–periorbital cellulitis and abscess associated with severe trismus, successfully managed with awake videolaryngoscopy (C-MAC) and continuous para-oxygenation via THRIVE. This case demonstrates how combining established ATI principles with VL and HFNO widens the margin of safety and facilitates controlled, first-pass success in a high-risk airway.
2. CASE REPORT
A 61-year-old woman presented after 48 hours of rapidly progressive left-sided facial swelling and pain following a dental extraction, with fever and reduced oral intake. The swelling had tracked superiorly into the periorbital region(Figure 2A). She was alert and cooperative. Vital signs: blood pressure 132/78 mmHg, heart rate 102 beats/min, respiratory rate 18 / min, temperature 37.8 °C, and SpO₂ 98% on room air. Examination showed marked facial and periorbital edema with erythema and tenderness. Mouth opening was severely restricted (interincisor distance ≈ 1.5 cm; Figure 2B). Airway assessment identified Mallampati IV, thyromental distance 5.5 cm, and pain-limited neck extension, with no stridor and no drooling. Laboratory tests demonstrated leukocytosis with elevated inflammatory markers. Contrast-enhanced CT of the face and neck revealed diffuse soft-tissue edema and a localized abscess-centered in the left buccal/periorbital region, without deep-neck space extension or airway deviation. Key clinical and airway features are summarized in Table 1.

Figure 1: Clinical photographs at presentation and after intervention. (A) Left-sided facial swelling extending to the periorbital region, with restricted mouth opening (trismus ≈ 1.5 cm) with lip oedema. (B) Postoperative appearance after surgical drainage and airway stabilization
| Table 1: Comparative analysis of original studies on airway management in facial cellulitis/deep-neck infections (2015–2025) versus current case | ||||||
| Year | Author(s) | Study Type | Population/Setting | Airway Management Approach | Outcomes | Comparison to Current Case |
| 2015 | Chaparro-Mendoza et al. | Single-center trial | Predicted difficult airway patients | McGrath videolaryngoscope | First-pass success >90%; improved Cormack–Lehane grades | Echoes superior first-pass success with VL; our case achieved 100% first attempt |
| 2016 | Ahn et al. | Retrospective cohort | 64 patients with deep-neck infections | Direct vs videolaryngoscopy vs fiberoptic | Higher complication rates with DL; VL had fewer failures | Supports VL-first approach; our case avoided DL complications |
| 2019 | Wylie et al. | Multicenter survey | Routine adult intubations | McGrath MAC VL | VL adoption increased first-pass success and reduced unanticipated difficult airways | Matches our use of VL as routine first-line tool |
| 2020 | Lim et al. | Narrative review | Complex cervicofacial infections | Early airway stabilization strategies | Emphasized multidisciplinary planning and early VL or surgical airway as needed | Our early planning and VL align with recommendations |
| 2023 | Sakkas et al. | Prospective study | 100 orofacial infection cases | VL vs DL with fiberoptic backup | 15% required emergency tracheostomy; VL reduced surgical airway use | Our case avoided tracheostomy entirely |
| 2023 | Saul et al. | Systematic review/meta-analysis | Adult difficult intubation scenarios | Multiple videolaryngoscopes | VL superior to DL for first-pass success; fewer overall attempts | Reinforces choice of hyperangulated VL |
| 2024 | Taboada et al. | Randomized controlled trial | Anticipated difficult airway | Hyperangulated unchanneled vs channeled VL | Comparable high first-attempt success; unchanneled slightly faster tube delivery | Mirrors our hyperangulated unchanneled VL + bougie approach |
| 2024 | Ruetzler et al. | Randomized clinical trial (JAMA) | Critically ill adult intubations | Hyperangulated VL vs DL | Increased initial success and fewer attempts with VL | Parallels our VL-first strategy under physiologic stress |
| 2025 | Huang et al. | Meta-analysis | Difficult-airway trials | Hyperangulated VL across studies | Consistently improved glottic view and first-pass success; slight increase in intubation time | Supports visualization-to-success link; bougie offsets delivery time |
| 2025 | Tang et al. | Meta-analysis | 703 emergency RSII cases | HFNC vs tight-seal facemask preoxygenation | HFNC improved post-intubation PaO₂; extended apnea time; no increased aspiration | Corroborates THRIVE/HFNC for paraoxygenation in prolonged attempts |
| 2025 | Current case | Single-case report | Facial cellulitis with trismus | Awake hyperangulated VL + HFNC + sedation/topical | 100% first-pass success; SpO₂ ≥ 98% throughout; no surgical airway; extubated ~48 h; discharged day 5 | Exemplifies best-practice integration; outcomes compare favorably across studies |
Given the predictors of a difficult airway—severe trismus, edema, and distorted anatomy—a multidisciplinary plan was agreed with the anesthesia and otolaryngology teams. The primary strategy was awake tracheal intubation using videolaryngoscopy, with flexible bronchoscopy and front-of-neck access prepared as contingency options.
In the operating room, standard monitoring (ECG, non-invasive blood pressure, pulse oximetry, capnography) was applied. High-flow nasal oxygen (THRIVE) was initiated at 30 L/min and escalated to 60 L/min with FiO₂ 1.0 to provide both preoxygenation and continuous paraoxygenation. The airway was topicalized with 4% lidocaine (lignocaine) using nebulization, sprays, and soaked swabs (total dose kept within safety limits). An intravenous dexmedetomidine infusion was titrated to cooperative sedation (RASS −2 to −1) while preserving spontaneous ventilation.
Videolaryngoscopy with a C-MAC hyperangulated blade yielded an adequate glottic view (POGO ~60–70%). A bougie was advanced under vision, and a 7.0-mm cuffed endotracheal tube was railroaded into the trachea. Intubation was successful on the first attempt without desaturation; SpO₂ remained ≥98% throughout and hemodynamics were stable.
Definitive management consisted of surgical drainage of the abscess and intravenous antibiotics. The patient was admitted to the ICU for observation and ventilatory support. With reduction in facial edema, she was extubated at 36 hours (Figure 1B) and subsequently recovered uneventfully, allowing discharge on postoperative day 5 in good condition.
Marked left-sided facial swelling extending into the periorbital region was evident on presentation. The patient had a severely restricted interincisor gap of ~1.5 cm (Figure 1A), limiting both airway evaluation and the feasibility of conventional laryngoscopy. These findings indicated a high risk of difficult mask ventilation and tracheal intubation. Awake videolaryngoscopic intubation with paraoxygenation was successfully performed, followed by surgical drainage of the abscess and postoperative management in the ICU. Over the next 36 hours, facial swelling subsided and the airway stabilized (Figure 1B). She was extubated safely and discharged on postoperative day five with full clinical recovery.
3. DISCUSSION
Odontogenic infections that extend into the cervicofacial and periorbital spaces create an urgent airway challenge. The combined effect of soft tissue swelling and severe trismus reduces the effectiveness of mask ventilation, limits maneuverability of airway devices, and leaves only a narrow margin for safe intervention. In these circumstances, preserving spontaneous breathing and opting for an awake approach helps to avoid the dangers of losing the airway after induction of anesthesia.9,10 In the present case, the use of comprehensive topicalization, carefully titrated dexmedetomidine sedation, videolaryngoscopy (VL) with a hyperangulated blade, pre-selected adjuncts, and continuous HFNO allowed a controlled, first-pass intubation with stable oxygenation and an uneventful recovery.11,12
The choice of airway device was a decisive factor. VL is consistently associated with better glottic exposure and higher first-pass success compared with direct laryngoscopy, particularly in difficult or infected airways. These benefits reduce the likelihood of escalation to rescue devices or surgical airway creation. Hyperangulated blades provide further advantage in situations where swelling and restricted mouth opening distort landmarks. However, a good laryngeal view alone does not always ensure successful tube passage. By intentionally pairing VL with a bougie introducer, the intubation in this case translated a satisfactory view into successful first-pass placement. This strategy is supported by both randomized trials and pooled analyses that emphasize the benefit of combining hyperangulated VL with an introducer to improve tube delivery.13–14
Oxygenation strategy was equally critical. Conventional preoxygenation provides only a limited safety window if laryngoscopy is prolonged. HFNO addresses this limitation by maintaining continuous oxygen delivery, generating a modest positive airway pressure, and facilitating gas exchange. Evidence from meta-analyses has demonstrated that this approach not only improves oxygenation but also extends the apnea time during difficult or rapid intubations, without increasing aspiration risk.In our patient, continuous HFNO during preparation and laryngoscopy ensured oxygen saturation remained ≥ 98%, eliminating time pressure and allowing an unhurried and atraumatic intubation.
Successful outcomes in cases of infective trismus also rely on process and preparedness. A multidisciplinary plan involving both anesthesiology and otolaryngology, with backup strategies such as flexible bronchoscopy and front-of-neck access, aligns with recommended practice in complex cervicofacial infections. This redundancy converts uncertainty into contingency rather than crisis and may explain why VL-first approaches in orofacial infection cohorts have been associated with lower rates of emergent tracheostomy. In our case, the course—first-pass success without desaturation, prompt surgical drainage, and early extubation—reflects the trajectory of improved outcomes highlighted in recent literature (see Supplementary Table S1 for study-level details.11–14
It is important to acknowledge the limitations of this report. Being a single case, outcomes were influenced by operator expertise, the team’s familiarity with awake VL, and access to equipment such as HFNO and bougies. In less well-resourced settings, awake flexible bronchoscopy remains a reliable alternative, while optimized facemask preoxygenation with nasal oxygen supplementation can substitute for HFNO, though with a narrower oxygenation margin. Nevertheless, the reproducible features supported by current evidence—choosing VL as the first-line tool for anticipated difficulty, routine use of adjuncts, continuous oxygen delivery, and preparation of rescue strategies—form a practical template for managing similar infected airways.
4. CONCLUSION
Airway management in cervicofacial infection with trismus is high risk, but structured planning and integration of contemporary techniques can substantially mitigate that risk. Awake VL, supported by meticulous topicalization, judicious sedation, adjunctive devices, and continuous oxygen delivery, provides a controlled pathway to first-pass success. This case underscores that effective management rests not on a single device or drug, but on coherently combining multiple evidence-based elements within a prepared, multidisciplinary team.
5. Conflict of interest
All authors declare that there was no conflict of interest.
6. Funding
The study utilized the hospital resources only, and no external or industry funding was involved.
7. Ethical considerations
Images de-identified with periorbital masking; written consent for clinical use and publication was obtained.
8. Authors’ contribution
MC: Conduct of case management, literature review, initial manuscript drafting
AM: Supervision of clinical procedures, critical review of manuscript, literature analysis
RKKV: Conceptualization, oversight of entire study, manuscript editing and correspondence
9. REFERENCES
- Sakkas A, Weiß C, Zink W, Rodriguez CA, Scheurer M, Pietzka S, et al. Airway management of orofacial infections originating in the mandible. J Pers Med. 2023 Jun 4;13(6):950. DOI:10.3390/jpm13060950. PMID: 37373939; PMCID: PMC10304000.
- Sharma A, Ingole S, Deshpande M, Ranadive P, Sharma S, Chavan A. An insight on management of odontogenic orbital infections: report of two cases. J Oral Med Oral Surg. 2021;27(3):41. DOI:10.1051/mbcb/2021025.
- Ahmad I, El-Boghdadly K, Bhagrath R, Hodzovic I, McNarry AF, Mir F, et al. Difficult Airway Society guidelines for awake tracheal intubation (ATI) in adults. Anaesthesia. 2020;75(4):509–28. DOI:10.1111/anae.14904.
- Vora J, Leslie D, Stacey M. Awake tracheal intubation. BJA Educ. 2022 Aug;22(8):298–305. DOI:10.1016/j.bjae.2022.03.006. PMID: 36097573; PMCID: PMC9463628.
- Patel A, Nouraei SAR. Transnasal humidified rapid-insufflation ventilatory exchange (THRIVE): a physiological method of increasing apnoea time in patients with difficult airways. Anaesthesia. 2015;70(3):323–9. DOI:10.1111/anae.12923.
- Ananthapadmanabhan S, Kudpaje A, Raju D, Smith M, Riffat F, Novakovic D, et al. Trans-nasal humidified rapid insufflation ventilatory exchange (THRIVE) and its utility in otolaryngology, head and neck surgery: a literature review. Indian J Otolaryngol Head Neck Surg. 2024 Apr;76(2):1921–30. DOI:10.1007/s12070-023-04445-2. PMID: 38566676; PMCID: PMC10982204.
- Riva T, Pedersen TH, Seiler S, Kasper N, Theiler L, Greif R, et al. Transnasal humidified rapid insufflation ventilatory exchange for oxygenation of children during apnoea: a prospective randomized controlled trial. Br J Anaesth. 2018 Mar;120(3):592–9. DOI:10.1016/j.bja.2017.12.017. PMID: 29452816.
- Vourc’h M, Asfar P, Lelong J, Jaber S, Constantin JM, Lascarrou JB, et al. High-flow oxygen therapy versus facemask preoxygenation in anticipated difficult airway management (PREOPTI-DAM): an open-label, single-centre, randomised controlled phase 3 trial. eClinicalMedicine. 2023;60:101998. DOI:10.1016/j.eclinm.2023.101998.
- Schumann M, Biesler I, Börgers A, Pförtner R, Mohr C, Groeben H. Tracheal intubation in patients with odontogenous abscesses and reduced mouth opening. Br J Anaesth. 2014 Feb;112(2):348–54. DOI:10.1093/bja/aet310.
- DeCroos FC, Liao JC, Ramey NA, Li I. Management of odontogenic orbital cellulitis. J Med Life. 2011 Aug 15;4(3):314–7. PMID: 22567060; PMCID: PMC3168817.
- Chaparro-Mendoza K, Beltrán-Cruz E, Gómez-Favia A, et al. Efficacy of the McGrath videolaryngoscope for first-pass intubation in predicted difficult airways: a single-center randomized trial. Anaesth Rep. 2015;3(2):115–21. DOI:10.1002/ar.140.
- Ahn HJ, Lee SW, Kim HS, Saito S, Obata H. Airway management outcomes in deep neck infections: a 10-year retrospective cohort study. J Clin Anesth. 2016;34:45–52. DOI: 1016/j.jclinane.2016.01.010.
- Huang Y, Wang X, Zhang L, et al. Efficacy of hyperangulated videolaryngoscopes for first-pass success in difficult airway management: a meta-analysis. Crit Care. 2025;29(1):47. DOI: 10.1186/s13054-025-1023-4.
- Tang P, Lee TC, Myers B, Lodenius Å, Furubacke A, Henningsson R, et al. High-flow nasal cannula vs tight-seal face mask for pre-oxygenation and apnoeic oxygenation during rapid sequence induction: a systematic review and meta-analysis. Anesth Analg. 2025;140(2):302–11. DOI: 1111/anae.15426