Sandeep Veer 1 , Reshma Salim 2 , Supriya Gholap 3 , Hashika Jani 4
Correspondence:
We report the case of a 54-year-old female with ESRD planned for cadaveric renal transplantation highlights the critical role of the anesthesiologist in managing perioperative challenges during renal transplantation in a patient with ischemic heart disease (IHD), diabetes mellitus (DM), and hypertension (HTN). It emphasizes the importance of a multidisciplinary approach, involving anesthesiologists, nephrologists, intensivists, and cardiologists, to optimize patient condition and ensure a successful surgical outcome. Renal transplantation, a standard treatment for end-stage renal disease (ESRD), requires careful anesthesia management, particularly in emergencies like cadaveric kidney transplants, where limited time for optimization poses additional risks. Preoperative assessment and risk mitigation are essential to minimizing complications and improving perioperative outcomes.
Keywords: kidney transplant; ESRD; intensivist; anesthesiologist
Citation: Veer S, Salim R, Gholap S, Jani H. Cardio-renal harmony: managing ischemic heart disease in renal transplantation. Anaesth. pain intensive care 2025;29(7):820-822. DOI: 10.35975/apic.v29i7.2980
Received: May 09, 2025; Revised: October 26, 2025; Accepted: January 01, 2025
The role of the anesthesiologist is crucial for the success of renal transplantation. This case report examines the anesthetic challenges during the perioperative management of a kidney recipient with ischemic heart disease (IHD), diabetes mellitus (DM), and hypertension (HTN) undergoing a cadaveric renal transplant. It underscores the collaborative efforts of anesthesiologists, nephrologists, intensivists, and cardiologists to optimize the patient's condition and ensure a successful surgical outcome. Managing anesthesia carefully in these cases is vital to improving perioperative results and minimizing complications.
Renal transplantation is a standard treatment for end-stage renal disease (ESRD), enhancing patients' quality of life and longevity.1-3 However, Patients undergoing cadaveric renal transplants occur as emergencies and thus less time is present for optimization. Preoperative optimization involves identifying and addressing risks to mitigate complications, as these recipients might have multiple comorbidities.4
This case highlights the anesthetic challenges encountered in a patient with IHD, DM, and HTN during a cadaveric renal transplant.4 Such patients are at increased risk of anemia, electrolyte imbalance, fluid overload, heart failure, and aspiration, in addition to being immunocompromised. Effective fluid management is crucial to avoid overload, and anemia should be monitored and treated to maintain adequate oxygen levels.5 Preventing aspiration through aspiration prophylaxis and careful airway management is essential.1 Immunocompromised patients require stringent infection control measures and adjustments in immunosuppressive therapy to protect against infections. These conditions necessitate a thorough and individualized approach to ensure patient safety and successful transplantation.36
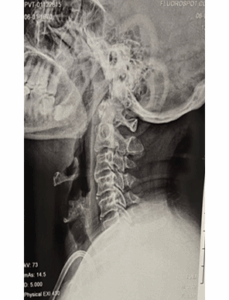
Figure 1: Radiologic examination of the vocal cords
We report a 54-year-old female with ESRD planned for cadaveric renal transplantation. The patient had suffered from uremic encephalopathy, for which she was on ventilatory support for a prolonged time and needed tracheostomy later. Since then, she had been on hemodialysis thrice weekly. Her comorbidities included diabetes for 25 years, managed with insulin aspart and insulin glargine, hypertension for 18 years, controlled with prazosin, nicardipine, isosorbide, and hydralazine, and clinical depression for 5 years, managed with antidepressants. Additionally, she had IHD for 4 years, underwent Percutaneous Transluminal Coronary Angioplasty (PTCA) with a drug-eluting stent, and took 75 mg of aspirin daily. She was also treated for extrapulmonary mediastinal tuberculosis 3 years ago.
eneral examination showed a moderately nourished, obese female, vitally stable with a post-tracheostomy scar over the midline of the neck. Investigations revealed old ischemic changes on ECG, including prominent Q waves and ST depression. A two-dimensional echocardiography revealed mild concentric left ventricular hypertrophy, an ejection fraction of 50%, trivial tricuspid regurgitation, and grade one diastolic dysfunction. High-resolution computed tomography of the thorax showed consolidation in the left lower lung's posterior segment, parenchymal bands in the bilateral lower zones, and the superior segment of the lower lung. Given these multiple conditions, a thorough preoperative assessment and collaboration among anesthesiologists, nephrologists, intensivists, and cardiologists were essential for optimizing the patient for surgery.
The risks associated with anesthesia and surgery were discussed with the patient and her relatives. Consent for ICU and ventilatory support, along with potential invasive procedures, was obtained. Antihypertensives were continued with cautious titration to avoid hypotension and maintain optimal renal perfusion. Strict glucose control was maintained perioperatively. An expert opinion was taken from the ENT side to evaluate the mobility of the vocal cords post-tracheostomy.
In the operating room, general anesthesia was induced with fentanyl (2 mcg/kg) and etomidate (0.3 mg/kg), followed by cis-atracurium (0.2 mg/kg). After preoxygenation with 100% O2 for three minutes, the airway was secured with a 7 mm endotracheal tube, intubation assisted by video laryngoscopy and 10% lignocaine sprayed to reduce the laryngoscopy response. Anesthesia maintenance involved oxygen, air, and isoflurane. Intraoperative fluid management was meticulously controlled to maintain euvolemia and prevent fluid overload, considering the patient's compromised cardiac function. Measures to minimize renal ischemia time and prevent further renal injury were prioritized, including adequate hydration and avoiding nephrotoxic agents.
The intraoperative period was uneventful. The patient was extubated and transferred to the ICU for close monitoring of vital signs and renal function. Her recovery was stable, with well-controlled cardiac function, blood glucose levels, and blood pressure. Post-transplant renal function showed improvement.
Anesthetic management of patients with IHD, DM, and HTN poses significant challenges due to factors such as poor left ventricular systolic function, ventricular enlargement, diabetic cardiomyopathy, and autonomic neuropathy.3 Advanced monitoring devices, like transesophageal echocardiography (TEE) and invasive BP monitoring, can assess ventricular function.1 ESRD patients often have a higher incidence of coronary artery disease (CAD), increasing morbidity and mortality. Altered pharmacodynamics and pharmacokinetics of anesthetic drugs, along with risks of fluid overload, LVH, and electrolyte imbalances, must be considered. Close monitoring of ABG and serum electrolytes is necessary, with particular attention to hyperkalemia. Adequate aspiration prophylaxis is also recommended to mitigate gastrointestinal risks.1
The challenge in this case was the post-tracheostomy status of the patient, so she may end up in difficulty. Other important considerations were perioperative management of input-output and blood sugar levels, optimal fluid management, and avoiding nephrotoxic drugs and drugs causing hyperkalemia, maintaining BP in a range of 150/90 mmHg, and avoiding drugs that increase the oxygen demand of the myocardium.
Renal transplantation is an intermediate-risk procedure, with transplant patients often being among the most complex. An extensive preoperative workup is essential for risk stratification and developing a tailored perioperative treatment plan.1
In conclusion, this case illustrates the successful perioperative management of a patient with IHD, DM, and HTN undergoing cadaveric renal transplantation. Although challenging, the process is highly rewarding when performed with meticulous attention to the pathophysiological changes associated with end-stage renal disease. A multidisciplinary approach involving anesthesiologists, nephrologists, cardiologists, and intensivists is crucial for achieving optimal outcomes. Careful preoperative assessment, vigilant intraoperative monitoring, and meticulous postoperative care are essential to optimize outcomes and minimize complications. Future research and guidelines may further refine the perioperative care of such complex patients, enhancing success rates in cadaveric renal transplants.6
Conflict of interest
All authors declare that there was no conflict of interest.
Authors’ contribution
All authors took part in the conduct of this case and the manuscript preparation.
Correspondence:
- Sandeep Veer, DR D. Y. Patil Medical College Hospital & Research Institute, Sant Tukaram Nagar, Pimpri, Pune 411018 Maharashtra, India; Email: drveersandeep@gmail.com
- Reshma Salim, DR D. Y. Patil Medical College Hospital & Research Institute, Sant Tukaram Nagar, Pimpri, Pune 411018 Maharashtra, India; Email: reshmasalim63@gmail.com
- Supriya Gholap, DR D. Y. Patil Medical College Hospital & Research Institute, Sant Tukaram Nagar, Pimpri, Pune 411018 Maharashtra, India; Email: supriyagholap123@gmail.com
- Hashika Jani, DR D. Y. Patil Medical College Hospital & Research Institute, Sant Tukaram Nagar, Pimpri, Pune 411018 Maharashtra, India; Email: hash.jani@gmail.com
ABSTRACT
We report the case of a 54-year-old female with ESRD planned for cadaveric renal transplantation highlights the critical role of the anesthesiologist in managing perioperative challenges during renal transplantation in a patient with ischemic heart disease (IHD), diabetes mellitus (DM), and hypertension (HTN). It emphasizes the importance of a multidisciplinary approach, involving anesthesiologists, nephrologists, intensivists, and cardiologists, to optimize patient condition and ensure a successful surgical outcome. Renal transplantation, a standard treatment for end-stage renal disease (ESRD), requires careful anesthesia management, particularly in emergencies like cadaveric kidney transplants, where limited time for optimization poses additional risks. Preoperative assessment and risk mitigation are essential to minimizing complications and improving perioperative outcomes.
Keywords: kidney transplant; ESRD; intensivist; anesthesiologist
Citation: Veer S, Salim R, Gholap S, Jani H. Cardio-renal harmony: managing ischemic heart disease in renal transplantation. Anaesth. pain intensive care 2025;29(7):820-822. DOI: 10.35975/apic.v29i7.2980
Received: May 09, 2025; Revised: October 26, 2025; Accepted: January 01, 2025
CASE REPORT
The role of the anesthesiologist is crucial for the success of renal transplantation. This case report examines the anesthetic challenges during the perioperative management of a kidney recipient with ischemic heart disease (IHD), diabetes mellitus (DM), and hypertension (HTN) undergoing a cadaveric renal transplant. It underscores the collaborative efforts of anesthesiologists, nephrologists, intensivists, and cardiologists to optimize the patient's condition and ensure a successful surgical outcome. Managing anesthesia carefully in these cases is vital to improving perioperative results and minimizing complications.
Renal transplantation is a standard treatment for end-stage renal disease (ESRD), enhancing patients' quality of life and longevity.1-3 However, Patients undergoing cadaveric renal transplants occur as emergencies and thus less time is present for optimization. Preoperative optimization involves identifying and addressing risks to mitigate complications, as these recipients might have multiple comorbidities.4
This case highlights the anesthetic challenges encountered in a patient with IHD, DM, and HTN during a cadaveric renal transplant.4 Such patients are at increased risk of anemia, electrolyte imbalance, fluid overload, heart failure, and aspiration, in addition to being immunocompromised. Effective fluid management is crucial to avoid overload, and anemia should be monitored and treated to maintain adequate oxygen levels.5 Preventing aspiration through aspiration prophylaxis and careful airway management is essential.1 Immunocompromised patients require stringent infection control measures and adjustments in immunosuppressive therapy to protect against infections. These conditions necessitate a thorough and individualized approach to ensure patient safety and successful transplantation.36

Figure 1: Radiologic examination of the vocal cords
We report a 54-year-old female with ESRD planned for cadaveric renal transplantation. The patient had suffered from uremic encephalopathy, for which she was on ventilatory support for a prolonged time and needed tracheostomy later. Since then, she had been on hemodialysis thrice weekly. Her comorbidities included diabetes for 25 years, managed with insulin aspart and insulin glargine, hypertension for 18 years, controlled with prazosin, nicardipine, isosorbide, and hydralazine, and clinical depression for 5 years, managed with antidepressants. Additionally, she had IHD for 4 years, underwent Percutaneous Transluminal Coronary Angioplasty (PTCA) with a drug-eluting stent, and took 75 mg of aspirin daily. She was also treated for extrapulmonary mediastinal tuberculosis 3 years ago.
eneral examination showed a moderately nourished, obese female, vitally stable with a post-tracheostomy scar over the midline of the neck. Investigations revealed old ischemic changes on ECG, including prominent Q waves and ST depression. A two-dimensional echocardiography revealed mild concentric left ventricular hypertrophy, an ejection fraction of 50%, trivial tricuspid regurgitation, and grade one diastolic dysfunction. High-resolution computed tomography of the thorax showed consolidation in the left lower lung's posterior segment, parenchymal bands in the bilateral lower zones, and the superior segment of the lower lung. Given these multiple conditions, a thorough preoperative assessment and collaboration among anesthesiologists, nephrologists, intensivists, and cardiologists were essential for optimizing the patient for surgery.
The risks associated with anesthesia and surgery were discussed with the patient and her relatives. Consent for ICU and ventilatory support, along with potential invasive procedures, was obtained. Antihypertensives were continued with cautious titration to avoid hypotension and maintain optimal renal perfusion. Strict glucose control was maintained perioperatively. An expert opinion was taken from the ENT side to evaluate the mobility of the vocal cords post-tracheostomy.
In the operating room, general anesthesia was induced with fentanyl (2 mcg/kg) and etomidate (0.3 mg/kg), followed by cis-atracurium (0.2 mg/kg). After preoxygenation with 100% O2 for three minutes, the airway was secured with a 7 mm endotracheal tube, intubation assisted by video laryngoscopy and 10% lignocaine sprayed to reduce the laryngoscopy response. Anesthesia maintenance involved oxygen, air, and isoflurane. Intraoperative fluid management was meticulously controlled to maintain euvolemia and prevent fluid overload, considering the patient's compromised cardiac function. Measures to minimize renal ischemia time and prevent further renal injury were prioritized, including adequate hydration and avoiding nephrotoxic agents.
The intraoperative period was uneventful. The patient was extubated and transferred to the ICU for close monitoring of vital signs and renal function. Her recovery was stable, with well-controlled cardiac function, blood glucose levels, and blood pressure. Post-transplant renal function showed improvement.
Anesthetic management of patients with IHD, DM, and HTN poses significant challenges due to factors such as poor left ventricular systolic function, ventricular enlargement, diabetic cardiomyopathy, and autonomic neuropathy.3 Advanced monitoring devices, like transesophageal echocardiography (TEE) and invasive BP monitoring, can assess ventricular function.1 ESRD patients often have a higher incidence of coronary artery disease (CAD), increasing morbidity and mortality. Altered pharmacodynamics and pharmacokinetics of anesthetic drugs, along with risks of fluid overload, LVH, and electrolyte imbalances, must be considered. Close monitoring of ABG and serum electrolytes is necessary, with particular attention to hyperkalemia. Adequate aspiration prophylaxis is also recommended to mitigate gastrointestinal risks.1
The challenge in this case was the post-tracheostomy status of the patient, so she may end up in difficulty. Other important considerations were perioperative management of input-output and blood sugar levels, optimal fluid management, and avoiding nephrotoxic drugs and drugs causing hyperkalemia, maintaining BP in a range of 150/90 mmHg, and avoiding drugs that increase the oxygen demand of the myocardium.
Renal transplantation is an intermediate-risk procedure, with transplant patients often being among the most complex. An extensive preoperative workup is essential for risk stratification and developing a tailored perioperative treatment plan.1
CONCLUSION
In conclusion, this case illustrates the successful perioperative management of a patient with IHD, DM, and HTN undergoing cadaveric renal transplantation. Although challenging, the process is highly rewarding when performed with meticulous attention to the pathophysiological changes associated with end-stage renal disease. A multidisciplinary approach involving anesthesiologists, nephrologists, cardiologists, and intensivists is crucial for achieving optimal outcomes. Careful preoperative assessment, vigilant intraoperative monitoring, and meticulous postoperative care are essential to optimize outcomes and minimize complications. Future research and guidelines may further refine the perioperative care of such complex patients, enhancing success rates in cadaveric renal transplants.6
Conflict of interest
All authors declare that there was no conflict of interest.
Authors’ contribution
All authors took part in the conduct of this case and the manuscript preparation.
REFERENCES
- Hyunjee Kim H, Jung H. Considerations regarding anesthesia for renal transplantation. Anesth Pain Med 2024;19:5-11 DOI: https://doi.org/10.17085/apm.23153\
- Parikh BK, Shah VR, Modi1 PR, Butala BP, Parikh GP. Anaesthesia for laparoscopic kidney transplantation: Influence of Trendelenburg position and CO2 pneumoperitoneum on cardiovascular, respiratory and renal function. Indian J Anaesth 2013 May;57(3):253-8. PMCID: PMC3748679 DOI: 4103/0019-5049.115607
- Aitken1E, Stevenson R, Hanif F, Raj D, Stevenson K, Kingsmore D. Renal Transplantation: An Update for Anaesthetists. Int J Anesthetic Anesthesiol 2016, 3:052 DOI: 23937/2377-4630/3/3/1052
- Tiwari P, Kulkarni A, Mathkar S. Anesthesia management of renal transplantation: A retrospective analysis, [Internet]. Indian J Clin Anaesth. 2021 [cited 2025 Oct 14];8(2):172-178. DOI 18231/j.ijca.2021.036
- Baxi V, Jain A, Dasgupta Anaesthesia for Renal Transplantation: An Update. Indian J Anaesth 2009;53 (2):139-147 PMCID: PMC2900097
- Bajwa SJS, Kulshrestha A. Anaesthesia considerations and challenges during renal transplantation: Current perspectives. Apollo Medicine 2012:9 (2);126-132. https://doi.org/10.1016/j.apme.2012.04.003